Ménière’s Disease Blog

When your inner ear puts your world on a roller coaster.
Think you may be experiencing dizziness, pressure in the ear, or fluctuating hearing? Learn more about Ménière’s disease, its symptoms, and available management options.

A Brief History: Who Was Prosper Ménière?
Dr. Prosper Ménière
Ménière’s Disease is named after Dr Prosper Ménière, a French physician and researcher who, in 1861, was among the first to connect vertigo and hearing loss to the inner ear.
Before Ménière’s observations, many believed these symptoms were linked to the brain. Prosper Ménière challenged this by suggesting that the inner ear, not the brain, was the source of these problems. His theory laid the foundation for modern audiovestibular medicine, and the condition now bears his name.
What Is Ménière’s Disease?
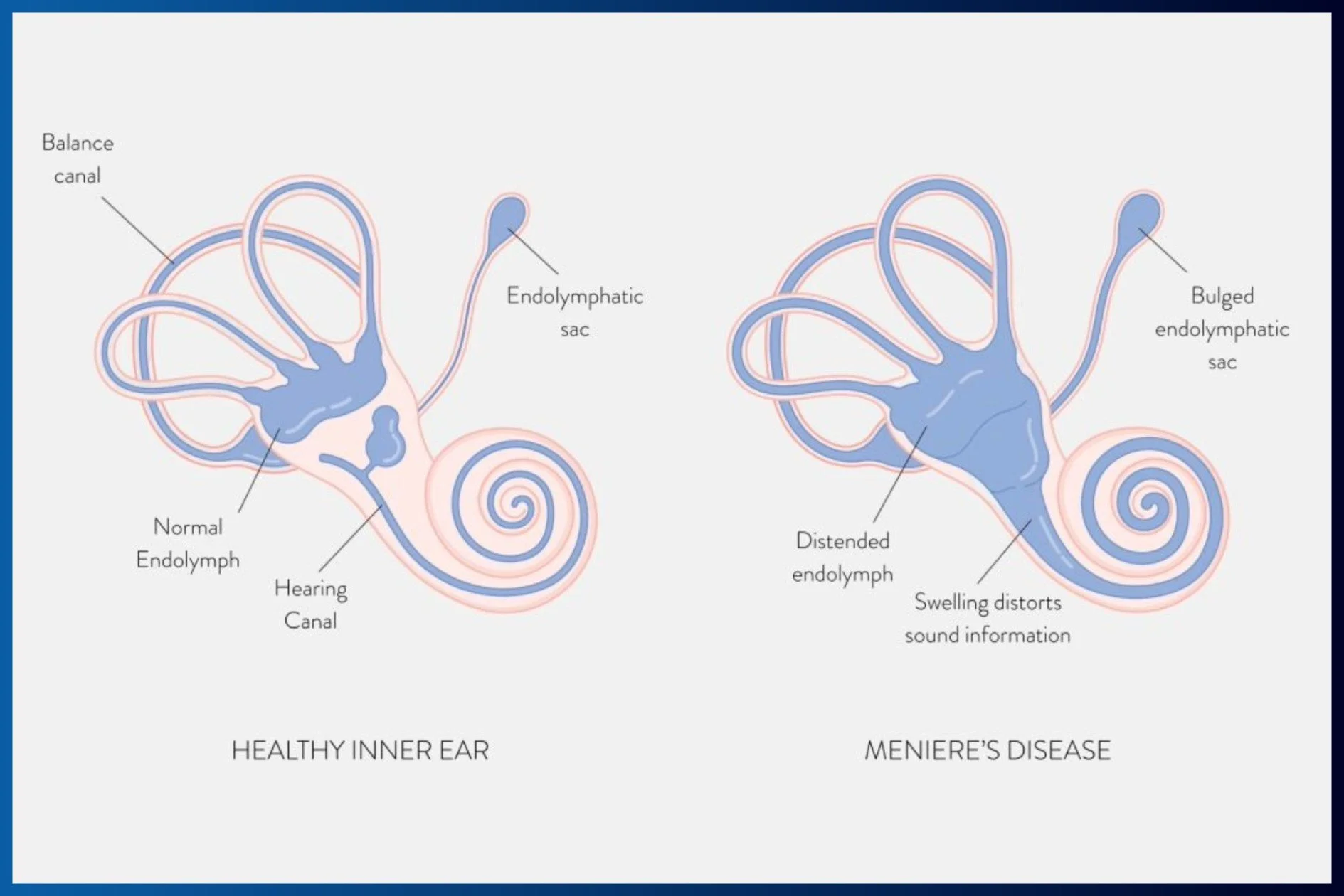
Ménière’s Disease is a chronic disorder of the inner ear, where abnormal fluid buildup disrupts your sense of balance and hearing. The symptoms come in episodes or attacks, which can vary in frequency and severity.
It most commonly affects adults between 40 and 60 years old, and while it usually starts in one ear, it can become bilateral in some cases over time.
Classic Symptoms of Ménière’s Disease

Vertigo
Sudden, strong spinning that can last 20 minutes to 12 hours, sometimes with nausea or vomiting. Can cause imbalance or falls.Fluctuating Hearing Loss
Hearing may go up and down, usually starts with low tones. Can become permanent if untreated.Tinnitus
Ringing, buzzing, or roaring sounds in the ear.Aural Fullness
Feeling of pressure or fullness in the ear.
What Causes It?
Ménière’s Disease is thought to be caused by excess fluid (called endolymph) in the labyrinth of the inner ear. This fluid buildup disrupts the delicate balance of signals that travel from the ear to the brain.
While the exact cause is unknown, possible contributors include:
Autoimmune disorders
Viral infections of the inner ear
Allergies
Head trauma
Genetics
Poor drainage or anatomical differences in the inner ear
Managing Ménière’s Disease
There’s no cure yet, but symptoms can be effectively managed. Treatment plans are tailored to each person’s lifestyle, severity of symptoms, and hearing profile.
1. Diet and Lifestyle
Low-sodium diet: Reduces inner ear fluid pressure
Avoiding caffeine, alcohol, and tobacco
Stress reduction: Stress can trigger attacks
2. Medications
Diuretics (water pills) to reduce fluid buildup
Anti-vertigo medications (e.g., meclizine) during attacks
Anti-nausea meds if vertigo leads to vomiting
3. Hearing Aids
For those with hearing loss or tinnitus
Advanced devices can provide relief from sound distortion and improve clarity
4. Vestibular Rehabilitation Therapy (VRT)
Tailored exercises that help the brain adapt to balance changes
5. Injection Therapy (less common)
Steroids injections in the middle ear.
Gentamicin injected into the ear in more severe cases.
6. Surgery (rare)
Endolymphatic sac surgery or vestibular nerve section for patients with disabling vertigo that doesn’t respond to other treatments.